Carbon Dioxide and Earth's Future: Pursuing the Prudent Path
6. Increased Human Mortality
The claim: Human mortality will escalate due to increasingly more severe and frequent heat waves, as well as a result of the enhanced spreading abroad of numerous vector-borne diseases, all brought about by CO2-induced global warming.
In exploring this sixth climate-alarmist claim, we examine the veracity of the prediction that rising temperatures will lead to future increases in human disease and death, beginning first with a discussion of correlations of human mortality with temperature followed by a brief discussion of viral and vector-borne diseases.
With respect to correlations of human mortality with temperature, Christidis et al. (2010) have written that "the IPCC AR4 states with very high confidence that climate change contributes to the global burden of disease and to increased mortality," citing the contribution of Confalonieri et al. (2007) to that document. In the NIPCC Report Climate Change Reconsidered (Idso and Singer, 2009), however, it is concluded that rising temperatures lead to a greater reduction in winter deaths than the increase they cause in summer deaths, resulting in a large net decrease in human mortality, based on findings described in the peer-reviewed scientific literature up through 2007. Thus, we here review only studies of the subject that have been published after that time, to see which viewpoint has ultimately prevailed.
In an effort handsomely suited to evaluate the supposedly very-high-confidence contention of the IPCC, Christidis et al. extracted the numbers of daily deaths from all causes reported on death registration data supplied by the UK Office of National Statistics for men and women fifty years of age or older in England and Wales for the period 1976-2005, which they divided by daily estimates of population that they obtained by fitting a fifth-order polynomial to mid-year population estimates, yielding deaths per million people, after which they compared the results with surface air temperature data that showed a warming trend during the same three-decade period of 0.47°C per decade. In addition, they employed a technique called optimal detection, which can be used to estimate the role played by human adaptation in the temperature-related changes in mortality they observed.
As expected, during the hottest portion of the year, warming led to increases in death rates, while during the coldest portion of the year it lead to decreases in death rates. But the real story is in the numbers. The three scientists report, for example, that if no adaptation had taken place, there would have been 1.6 additional deaths per million people per year due to warming in the hottest part of the year over the period 1976-2005, but there would have been 47 fewer deaths per million people per year due to warming in the coldest part of the year, for a lives-saved to life-lost ratio of 29.4, which represents a huge net benefit of the warming experienced in England and Wales over the three-decade period of warming. And when adaptation was included in the analysis, as was the case in the data they analyzed, they found there was only 0.7 of a death per million people per year due to warming in the hottest part of the year, but a decrease of fully 85 deaths per million people per year due to warming in the coldest part of the year, for a phenomenal lives-saved to life-lost ratio of 121.4. Clearly, therefore, the IPCC's "very-high-confidence" conclusion is woefully wrong. Warming is highly beneficial to human health, even without any overt adaptation to it. And when adaptations are made, warming is incredibly beneficial in terms of lengthening human life span.
Working in the Castile-Leon region of Spain -- a plateau in the northwestern part of the country that includes nine provinces with a low population density that can be considered as ageing -- Fernandez-Raga et al. (2010) obtained (from the country's National Meteorological Institute) meteorological data from weather stations situated in eight of the provincial capitals that covered the period 1980-1998, while they obtained contemporary mortality data from the country's National Institute for Statistics for deaths associated with cardiovascular, respiratory and digestive system diseases.
Various analyses of the monthly-averaged data revealed a number of interesting results. First, for all three of the disease types studied, the three researchers found that "the death rate is about 15% higher on a winter's day than on a summer's day," which they describe as "a result often found in previous studies," citing the work of Fleming et al. (2000), Verlato et al. (2002), Grech et al. (2002), Law et al. (2002) and Eccles (2002). And second, in a finding that helps to explain the first finding, the three researchers discovered that when monthly-averaged human death rates were plotted against monthly-averages of daily mean, maximum and minimum air temperature, the results nearly always took the form of a U-shaped concave parabola, as shown in the figure below.
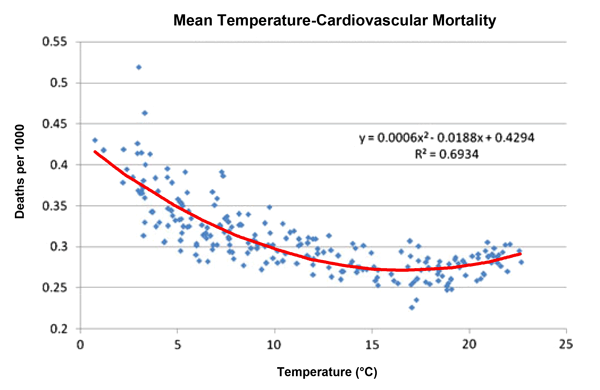
Monthly deaths in the Castile-Leon region of Spain attributable to cardiovascular disease vs. mean daily air temperature. Adapted from Fernandez-Raga et al. (2010).
For all three disease types, they found that all three temperatures (daily mean, maximum and minimum) at which minimum death rates occurred -- which they refer to as ideal or comfort temperatures -- were all within about 1-7°C of the maximum values typically reached by those three types of temperature, while they were anywhere from 14-24°C away from their minimum values. Consequently, the ideal or comfort temperatures were always very close to (and sometimes nearly identical to) the maximum values reached by the mean, maximum and minimum temperatures experienced in the region, while they were much more removed from the minimum values of those three temperature parameters, as illustrated in the figure above.
The data of this figure clearly demonstrate that the people of the Castile-Leon region of Spain are much more likely to die from a cardiovascular disease in the extreme cold of winter than in the extreme heat of summer. And the same was found to hold true with respect to dying from respiratory and digestive system diseases. Indeed, cold has been found to be a much greater killer of people than heat almost everywhere in the world, and in conjunction with almost any type of illness.
In a more broad-based study, Analitis et al. (2008) wrote that "in recent years, the effects of meteorologic factors on health have attracted renewed interest because of the observed and predicted climate change, which is expected to result in a general rise in temperature." And this development, in their words, has led to a "recent focus on heat-wave episodes," which may have fostered the perception that cold-related mortality is not as important a public health concern as is heat-related mortality.
To rectify this situation, the fourteen researchers analyzed short-term effects of cold weather on mortality in 15 European cities (Athens, Greece; Barcelona, Spain; Budapest, Hungary; Dublin, Ireland; Helsinki, Finland; Ljubljana, Slovenia; London, United Kingdom; Milan, Italy; Paris, France; Prague, Czech Republic; Rome, Italy; Stockholm, Sweden; Turin, Italy; Valencia, Spain; and Zurich, Switzerland). More specifically, they assessed the effects of minimum apparent temperature on cause- and age-specific daily mortality over the cold half of the year (October-March), using data from 1990-2000 that they analyzed via "Poisson regression and distributed lag models, controlling for potential confounders."
The international team of scientists -- hailing from Finland, Greece, Ireland, Italy, Slovenia, Spain and Sweden -- found that "a 1°C decrease in temperature was associated with a 1.35% increase in the daily number of total natural deaths and a 1.72%, 3.30% and 1.25% increase in cardiovascular, respiratory, and cerebrovascular deaths, respectively." In addition, they report that "the increase was greater for the older age groups," and that the cold effect "persisted up to 23 days, with no evidence of mortality displacement," which latter finding is extremely important, because in the case of heat-related deaths there is such a displacement, and its impact is huge.
In Germany, for example, Laschewski and Jendritzky (2002) analyzed daily mortality rates in Baden-Wurttemberg (10.5 million inhabitants) over the 30-year period 1958-97 to determine the sensitivity of the population of this moderate climatic zone to long- and short-term episodes of heat and cold. Their research indicated that mortality showed "a marked seasonal pattern with a minimum in summer and a maximum in winter." With respect to short-term exposure to heat and cold, however, they found that "cold spells lead to excess mortality to a relatively small degree, which lasts for weeks," and that "the mortality increase during heat waves is more pronounced, but is followed by lower than average values in subsequent weeks," which suggests, in their words, that people who died from short-term exposure to heat "would have died in the short term anyway."
With respect to this short-term mortality displacement that occurs in conjunction with heat-related deaths, Laschewski and Jendritzky's data demonstrate that it is precisely that, i.e., merely a displacement of deaths and not an overall increase. They found, for example, that the mean duration of above-normal mortality for the 51 heat episodes that occurred from 1968 to 1997 was 10 days, with a mean increase in mortality of 3.9%, after which there was a mean decrease in mortality of 2.3% for 19 days. Hence, the net effect of the two perturbations was actually an overall decrease in mortality of 0.2% over the full 29-day period. Consequently, it should be abundantly clear that cold spells are much more deadly than heat waves, and that we could thus expect global warming to confer significant benefits upon mankind by significantly reducing the very real killing power of routine bouts of colder-than-normal weather. And thus it was that Analitis et al. concluded their paper by stating that their results "add evidence that cold-related mortality is an important public health problem across Europe and should not be overlooked by public health authorities because of the recent focus on heat-wave episodes."
In providing some background for another recent study of the subject, Young and Kakinen (2010) write that "Arctic populations, especially indigenous people, could be considered as 'vulnerable,' because their health status generally shows disparities when compared to the national or more southern populations," and they say that "it is not known if the harsh climate, and especially cold temperatures, could be a contributing or causative factor of the observed health inequalities." Thus, to seek answers relative to this uncertainty, the two researchers determined mean January and July temperatures for 27 Arctic regions, based on weather station data for the period 1961-1990, as well as their association with a variety of health outcomes assessed by correlation and multiple linear regression analyses.
Following this protocol, the two researchers found that mean January temperature correlated negatively with several health outcomes, including infant mortality rate, age-standardized mortality rates (all causes), perinatal mortality rate and tuberculosis incidence rate, but that it correlated positively with life expectancy. That is to say, as mean January temperature rose, the desirable metric of life expectancy at birth rose right along with it, while all of the undesirable health metrics (such as mortality and disease incidence) declined. For example, they report that "for every 10°C increase in mean January temperature, the life expectancy at birth among males increased by about six years," while "infant mortality rate decreased by about four deaths per thousand live births."
As a result of their several findings, Young and Kakinen concluded that the cold climate of the Arctic is "significantly associated with higher mortality" and "should be recognized in public health planning," noting that "within a generally cold environment, colder climate results in worse health." For people living in these regions, therefore, a little global warming could go a long way towards improving their quality of life ... as well as the length of time they have to enjoy it!
In another impressive study, Deschenes and Moretti (2009) analyzed the relationship between weather and mortality, based on data that included the universe of deaths in the United States over the period 1972-1988, wherein they matched each death to weather conditions on the day of death and in the county of occurrence. These high-frequency data and the fine geographical detail then allowed them to estimate with precision the effect of cold and hot temperature shocks on mortality, as well as the dynamics of such effects, most notably, the existence or non-existence of a "harvesting effect," whereby the temperature-induced deaths either are or are not subsequently followed by a drop in the normal death rate, which could either partially or fully compensate for the prior extreme temperature-induced deaths.
The two researchers stated that their results "point to widely different impacts of cold and hot temperatures on mortality." In the latter case, they discovered that "hot temperature shocks are indeed associated with a large and immediate spike in mortality in the days of the heat wave," but that "almost all of this excess mortality is explained by near-term displacement," so that "in the weeks that follow a heat wave, we find a marked decline in mortality hazard, which completely offsets the increase during the days of the heat wave," such that "there is virtually no lasting impact of heat waves on mortality."
In the case of cold temperature days, they also found "an immediate spike in mortality in the days of the cold wave," but they report that "there is no offsetting decline in the weeks that follow," so that "the cumulative effect of one day of extreme cold temperature during a thirty-day window is an increase in daily mortality by as much as 10%." In addition, they say that "this impact of cold weather on mortality is significantly larger for females than for males," but that "for both genders, the effect is mostly attributable to increased mortality due to cardiovascular and respiratory diseases."
In further discussing their findings, Deschenes and Moretti state that "the aggregate magnitude of the impact of extreme cold on mortality in the United States is large," noting that it "roughly corresponds to 0.8% of average annual deaths in the United States during the sample period." And they estimate that "the average person who died because of cold temperature exposure lost in excess of ten years of potential life," whereas the average person who died because of hot temperature exposure likely lost no more than a few days or weeks of life. Hence, it is clear that climate-alarmist concerns about temperature-related deaths are wildly misplaced, and that halting global warming -- if it could ever be done -- would lead to more thermal-related deaths, because continued warming, which is predicted to be greatest in earth's coldest regions, would lead to fewer such fatalities.
Interestingly, the two scientists additionally report that many people in the United States have actually taken advantage of these evident facts by moving "from cold northeastern states to warm southwestern states." Based on their findings, for example, they calculate that "each year 4,600 deaths are delayed by the changing exposure to cold temperature due to mobility," and that "3% to 7% of the gains in longevity experienced by the U.S. population over the past three decades are due to the secular movement toward warmer states in the West and the South, away from the colder states in the North."
Working in the Southern Hemisphere, Bi et al. (2008) used correlation and autoregressive integrated moving average regression analyses to derive relationships between various aspects of weather and mortality in the general population and elderly (65 years of age and older) of Brisbane, Australia -- which they describe as having a subtropical climate -- over the period 1986-1995. In doing so, they determined that "death rates were around 50-80 per 100,000 in June, July, and August [winter], while they were around 30-50 per 100,000 in the rest of the year, including the summer," and that "this finding applied both to the general population and to the elderly population, and to deaths from various causes."
In discussing the fact that "more deaths occurred in the winter than during other seasons of the year, although winter in Brisbane is very mild," the researchers noted that "it is understandable that more deaths would occur in winters in cold or temperate regions, but even in a subtropical region, as indicated in this study, a decrease in temperatures (in winters) may increase human mortality." Consequently, the evidence continues to grow that extremes of cold lead to the deaths of many more people than extremes of heat in both cold and warm climates.
In a study with a slightly different take on the subject, Tam et al. (2009) studied daily mortality data from 1997 to 2002, which they obtained from the Hong Kong Census and Statistics Department, examining the association between diurnal temperature range (DTR = daily maximum temperature minus daily minimum temperature), while focusing on cardiovascular disease among the elderly (people aged 65 and older). And in doing so, they discovered "a 1.7% increase in mortality for an increase of 1°C in DTR at lag days 0-3," which results they describe as being "similar to those reported in Shanghai."
In discussing their findings, the four Hong Kong researchers stated that "a large fluctuation in the daily temperature -- even in a tropical city like Hong Kong -- has a significant impact on cardiovascular mortality among the elderly population." In addition, we note that it has long been known that the DTR has declined significantly over many parts of the world as mean global temperature has risen over the past several decades (Easterling et al., 1997), which is perhaps another reason why colder temperatures are a much greater risk to human life than are warmer temperatures, i.e., because as the planet warms, local DTRs tend to decline, which leads to a corresponding decline in human death rates.
Turning to the Shanghai study mentioned by Tam et al., we find that Cao et al. (2009) -- working within the nine urban districts of Shanghai, China -- used time-series and case-crossover approaches to assess the relationship between DTR and coronary heart disease (CHD) deaths that occurred between 1 January 2001 and 31 December 2004, based on mortality data for elderly people (66 years of age or older) that they obtained from the Shanghai Municipal Center of Disease Control and Prevention, plus temperature data they obtained from a fixed-site station in the Xuhui District of Shanghai, which they adjusted to account for the mortality impacts of long-term and seasonal trends in CHD mortality, day of week, temperature, relative humidity and concomitant atmospheric concentrations of PM10, SO2, NO2 and O3, which they obtained from the Shanghai Environmental Monitoring Center.
This work revealed, in Cao et al.'s words, that "a 1°C increase in DTR (lag = 2) corresponded to a 2.46% increase in CHD mortality on time-series analysis, a 3.21% increase on unidirectional case-crossover analysis, and a 2.13% increase on bidirectional case-crossover analysis," and that "the estimated effects of DTR on CHD mortality were similar in the warm and cool seasons." Thus, the seven scientists concluded that their data suggested that even "a small increase in DTR is associated with a substantial increase in deaths due to CHD." And since the DTR has declined significantly over most of the world as mean global air temperature has risen over the past several decades, it can be appreciated that the global warming with which this DTR decrease is associated (which is driven by the fact that global warming is predominantly caused by an increase in daily minimum temperature) has likely helped to significantly reduce the CHD-induced mortality of elderly people worldwide.
In one final study dealing with the heart, and employing a generalized additive statistical model that blends the properties of generalized linear models with additive models, Bayentin et al. (2010) analyzed the standardized daily hospitalization rates for ischemic heart disease (IHD) and their relationship with climatic conditions up to two weeks prior to the day of admission -- controlling for time trends, day of the season, and gender -- in order to determine the short-term effects of climate conditions on the incidence of IHD over the 1989-2006 time period for 18 different health regions of Quebec. Perhaps the most interesting and important finding of this study was, as they describe it, the fact that "a decline in the effects of meteorological variables on IHD daily admission rates was observed over the period of 1989-2006," which response, in their words, "can partly be explained by the changes in surface air temperature," which they describe as warming "over the last few decades," as is further described by Bonsal et al. (2001) and Zhang et al. (2000) for the 20th-century portion of the study's duration. In addition, they note that "winters have been steadily warmer," while "summers have yet to become hotter for most regions," which is another beneficial characteristic of the warming that was experienced over most of the planet throughout the latter part of the 20th century: a gradual reduction in DTR, as confirmed by the work of Easterling et al. (1997).
With respect to viral and vector-borne diseases, in a review of the pertinent literature that describes "those mechanisms that have led to an increase of virus activity in recent years," Zell et al. (2008) say "it is assumed that global warming is forced by the anthropogenic release of 'greenhouse gases'," and that a further "consistent assumption" has been a consequent "increased exposure of humans to tropical pathogens and their vectors." However, they note "there is dissent about this hypothesis (Taubes, 1997; Reiter, 2001; Hay et al., 2002; Reiter et al., 2003; Randolph, 2004; Zell, 2004; Halstead, 2008)," and they thus go on to explore it in more detail, ultimately concluding that "only very few examples point toward global warming as a cause of excess viral activity." Instead, they find that "coupled ocean/atmosphere circulations and continuous anthropogenic disturbances (increased populations of humans and domestic animals, socioeconomic instability, armed conflicts, displaced populations, unbalanced ecosystems, dispersal of resistant pathogens etc.) appear to be the major drivers of disease variability," and that global warming "at best" merely "contributes."
Also exploring this issue about the same time were Gage et al. (2008), who reviewed what was then known about it; and in doing so, the four researchers -- all of whom hail from the U.S. Centers for Disease Control's National Center for Zoonotic, Vector-Borne, and Enteric Diseases -- concluded that "the precise impacts" of the various climatic changes that are typically claimed to occur in response to rising atmospheric CO2 concentrations "are difficult to predict." Indeed, they say that "in some areas, climate change could increase outbreaks and the spread of some vector-borne diseases while having quite the opposite effect on other vector-borne diseases."
In further discussing this complex situation, they also wrote that "the mere establishment of suitable vectors for a particular agent does not necessarily mean that spread to humans will commonly occur, as indicated by the limited transmission of dengue and malaria in the southern U.S.," because, as they continue, "local transmission has been limited by factors unrelated to the climatic suitability of the areas for the relevant vector species." And they add that "in instances where a vector-borne disease is also zoonotic, the situation is even more complex, because not only must the vector and pathogen be present, but a competent vertebrate reservoir host other than humans must also be present."
So what are some of the non-climatic factors that impact the spread of vector-borne diseases of humans? Gage et al. list "many other global changes concurrently transforming the world, including increased economic globalization, the high speed of international travel and transport of commercial goods, increased population growth, urbanization, civil unrest, displaced refugee populations, water availability and management, and deforestation and other land-use changes," as well, we would add, as the many different ways in which these phenomena are dealt with by different societies.
Unfortunately, there is almost no way to correctly incorporate such factors into models to correctly forecast disease incidence in the future. Therefore, in light of the many complex phenomena that concurrently impact the spread of vector-borne diseases, it is clearly unjustified to claim that any future warming of the globe will necessarily lead to a net increase in their global incidence, for just the opposite could well be true, depending on the type and degree of a number of current and potential societal impacts on the world of nature, as well as the diverse natures of the evolving states of the planet's multiple human societies.
Contemporaneously -- and noting that "dengue is a spectrum of disease caused by four serotypes of the most prevalent arthropod-borne virus affecting humans today," and that "its incidence has increased dramatically in the past 50 years," to where "tens of millions of cases of dengue fever are estimated to occur annually, including up to 500,000 cases of the life-threatening dengue hemorrhagic fever/dengue shock syndrome" -- Kyle and Harris (2008) conducted a review of the pertinent scientific literature, exploring "the human, mosquito, and viral factors that contribute to the global spread and persistence of dengue, as well as the interaction between the three spheres, in the context of ecological and climate change." So what did they learn?
With respect to the status of dengue fever within the context of climate change, the two researchers say "there has been a great deal of debate on the implications of global warming for human health," but that "at the moment, there is no consensus." However, in the case of dengue, they say "it is important to note that even if global warming does not cause the mosquito vectors to expand their geographic range, there could still be a significant impact on transmission in endemic regions," as they report that "a 2°C increase in temperature would simultaneously lengthen the lifespan of the mosquito and shorten the extrinsic incubation period of the dengue virus, resulting in more infected mosquitoes for a longer period of time." Nevertheless, they note there are "infrastructure and socioeconomic differences that exist today and already prevent the transmission of vector-borne diseases, including dengue, even in the continued presence of their vectors." Consequently, it would appear that whatever advantages rising temperatures might possibly confer upon the dengue virus vector, they can be more than overcome by proper implementation of modern vector control techniques.
One year later, Russell (2009) -- a Professor in the Department of Medicine of the University of Sydney and founding Director of its Department of Medical Entomology -- reported that "during the past 10 years, there has been increasing concern for health impacts of global warming in Australia, and continuing projections and predictions for increasing mosquito-borne disease as a result of climate change." However, he stated that these claims "are relatively simplistic, and do not take adequate account of the current or historic situations of the vectors and pathogens, and the complex ecologies that might be involved," after which he went on to review the consequences of these several inadequacies for malaria, dengue fever, the arboviral arthritides (Ross River and Barmah Forest viruses) and the arboviral encephalitides (Murray Valley encephalitis and Kunjin viruses). This he did within the context of predictions that have been made for projected climate changes as proposed and modeled by Australia's Commonwealth Scientific and Industrial Research Organization and the Intergovernmental Panel on Climate Change. What he concluded from this review was that "there might be some increases in mosquito-borne disease in Australia with a warming climate, but with which mosquitoes and which pathogens, and where and when, cannot be easily discerned." Therefore, the strongest statement he could make was that "of itself, climate change as currently projected, is not likely to provide great cause for public health concern with mosquito-borne disease in Australia."
In another paper, Russell et al. (2009) wrote that "dengue has emerged as a leading cause of morbidity in many parts of the tropics," noting that "Australia has had dengue outbreaks in northern Queensland." In addition, they reported that "substantial increases in distribution and incidence of the disease in Australia are projected with climate change," or, more specifically, "with increasing temperatures." Hence, they explored the soundness of these projections by reviewing pertinent facts about the history of dengue in Australia, determining that the dengue vector (the Aedes aegypti mosquito) "was previously common in parts of Queensland, the Northern Territory, Western Australia and New South Wales," and that it had, "in the past, covered most of the climatic range theoretically available to it," adding that "the distribution of local dengue transmission has [historically] nearly matched the geographic limits of the vector."
This being the case, the six scientists concluded that the vector's current absence from much of Australia, as Russell et al. described it, "is not because of a lack of a favorable climate." Thus, they reasoned that "a temperature rise of a few degrees is not alone likely to be responsible for substantial increases in the southern distribution of A. aegypti or dengue, as has been recently proposed." Instead, they reminded everyone that "dengue activity is increasing in many parts of the tropical and subtropical world as a result of rapid urbanization in developing countries and increased international travel, which distributes the viruses between countries." Rather than futile attempts to limit dengue transmission by controlling the world's climate, therefore, the medical researchers recommended that "well resourced and functioning surveillance programs, and effective public health intervention capabilities, are essential to counter threats from dengue and other mosquito-borne diseases."
Studying dengue simultaneously in three other parts of the world, Johansson et al. (2009) wrote that "mosquito-borne dengue viruses are a major public health problem throughout the tropical and subtropical regions of the world," and that "changes in temperature and precipitation have well-defined roles in the transmission cycle and may thus play a role in changing incidence levels." Therefore, as they continued, since "the El Niño Southern Oscillation (ENSO) is a multiyear climate driver of local temperature and precipitation world wide," and since "previous studies have reported varying degrees of association between ENSO and dengue incidence," as they describe it, they decided to analyze "the relationship between ENSO, local weather, and dengue incidence in Puerto Rico, Mexico, and Thailand, which they did by searching for relationships between ENSO, local weather and dengue incidence in Puerto Rico (1986-2006), Mexico (1985-2006), and Thailand (1983-2006), using wavelet analysis as a tool to identify time- and frequency-specific associations.
As a result of these activities, the three researchers reported that they "did not find evidence of a strong, consistent relationship in any of the study areas," while Rohani (2009), who wrote a Perspective piece on their study, stated that they found "no systematic association between multi-annual dengue outbreaks and El Niño Southern Oscillation." Thus, as included in the Editors' Summary of Johansson et al.'s paper, their findings provided "little evidence for any relationship between ENSO, climate, and dengue incidence." And in light of the inconclusive nature of Johansson et al.'s analysis, there still remains a lack of substantive real-world support for the climate-alarmist claim that global warming promotes the global intensification and spread of the spectrum of diseases caused by the different serotypes of the family of dengue viruses.
In still another review paper dealing with the possible impacts of climate change on the spread of infectious diseases, Randolph (2009) wrote that it is generally tacitly assumed -- and even explicitly stated -- that climate change will result only in a worsening of the situation, with the expansion of vector-borne diseases into higher latitudes and an increased disease incidence. In fact, she states that implicit in almost all of the literature on this subject -- both popular and scientific -- "is an assumption that environmental change is more likely to strengthen the transmission potential and expand the range, rather than to disrupt the delicate balance between pathogen, vector and host upon which these systems depend."
With this background, the zoologist from the UK's University of Oxford explores the evidence for these two opposing world views via an analysis of what the bulk of the accurately-informed scientific literature on the subject seems to suggest. In doing so, she finds that "the mercurial epidemiology of each vector-borne disease is the system-specific product of complex, commonly nonlinear, interactions between many disparate environmental factors," which include "not only climate but also other abiotic conditions (e.g., land cover) and the physical structure of the environment (e.g., water sources), and further biotic factors such as host abundance and diversity." She additionally indicates that a number of socioeconomic factors drive human living conditions and behaviors that determine the degree of exposure to the risk posed to them, and that nutritional status and concomitant immunity also determine the degree of resistance to infection.
In some interesting examples from the past, Randolph notes that the upsurge of tick-borne diseases within preexisting endemic regions in central and Eastern Europe "appears to be an unforeseen consequence of the fall of the iron curtain and the end of the cold war," which she describes as "a sort of political global warming." Also noted is the fact that "the introduction of the mosquito Aedes aegypti to the Americas within water containers on board slave ships from Africa was repeated four centuries later by the dispersal of the Asian tiger mosquito, A. albopictus, from Japan to the United States within water trapped in used car tires (Hawley et al., 1987; Reiter and Sprenger, 1987)."
This phenomenon, according to Randolph, continues today, augmented by trade in other water-carrying goods such as Asian Luck Bamboo plants, which activities have allowed this mosquito species "to establish itself in almost all New World countries, a dozen European countries, parts of West Africa, and the Middle East." All of these disease expansions, in her words, have "nothing to do with climate change," which also holds true for such chance events as "the introduction of West Nile virus into New York in 1999, most probably by air from Israel (Lanciotti et al., 1999)," and the introduction "of the BTV-8 strain of bluetongue virus into the Netherlands in 2006 from South Africa (Saegerman et al., 2008)."
In concluding her brief treatise, Randolph states that the real-world complexity within each disease system emphasizes that "any expectation of a simple consistent response to climate change, i.e., a universal worsening of the situation, is ill founded," noting further that "there is no single infectious disease whose increased incidence over recent decades can be reliably attributed to climate change." Consequently, she says that "if the purpose of predictions about the future is to guide policy and therefore government spending, exaggerated simplistic rhetoric about the universality and uniformity of the impact of climate change on infectious disease risk is morally indefensible," especially "if it distracts public health agencies from more effective ameliorative action targeted at the real causes."
Contemporaneously, Harvell et al. (2009) stated that "in temperate climates, we might expect the range and activity of mosquitoes and the pathogens they vector, such as malaria and dengue, to increase with warmer temperatures." However, "from a later vantage point in 2009," they indicated that "surprisingly, insect-vectored diseases resoundingly do not show a net expansion in range or increase in prevalence." As for why this was so, the five scientists gave three explanations that they attributed to Lafferty (2009a): "(1) anthropogenic activities directly influence the distributions of vectors and infectious disease in ways unrelated to climate, (2) vectors and pathogens are limited by thermal maxima, so that temperature changes lead to shifts rather than expansions in distribution, and (3) other factors such as host acquired immunity and vector or parasite life history traits are linked to habitat suitability in addition to climate." In addition, they noted the important role that may be played by "evolutionary changes in properties of the host or pathogen," and in concluding their paper they therefore wrote that "ecologists need to consider how host biology, including movement behavior and acquired immunity, can mediate the impacts of global change on parasite/pathogen dynamics and disease severity," because, as they concluded, "at present, many of these mechanisms are poorly known."
Turning directly to the Lafferty (2009a) paper, we again read that climate-alarmist "wisdom" holds that "global climate change will result in an expansion of tropical diseases, particularly vector-transmitted diseases, throughout temperate areas," examples of which include "schistosomiasis (bilharzia or snail fever), onchocerciasis (river blindness), dengue fever, lymphatic filariasis (elephantiasis), African trypanosomiasis (sleeping sickness), leishmaniasis, American trypanosomiasis (Chagas disease), yellow fever, and many less common mosquito and tick-transmitted diseases of humans," as well as many diseases of "nonhuman hosts." In a critique of this alarmist point of view, based on his review of the scientific literature, he concludes that "while climate has affected and will continue to affect habitat suitability for infectious diseases, climate change seems more likely to shift than to expand the geographic ranges of infectious diseases," and that "many other factors affect the distribution of infectious disease, dampening the proposed role of climate." In fact, he concludes that "shifts in climate suitability might actually reduce the geographic distribution of some infectious diseases." And of perhaps even greater importance (because it is a real-world observation), he reports that "although the globe is significantly warmer than it was a century ago, there is little evidence that climate change has already favored infectious diseases."
In a companion paper (Lafferty, 2009b), the U.S. researcher lists a number of ways in which ecologists "can contribute substantially to the general theory of climate and infectious disease," some of the most important of which have to deal with "[1] multiple hosts and parasite species (Dobson, 2009), [2] nonhuman hosts (Harvell et al., 2009), [3] accounting for the effects of immunity (Dobson, 2009; Harvell et al., 2009; Ostfeld, 2009; Pascual and Bouma, 2009), [4] quality and details of [4a] climatic data and [4b] appropriate measures of disease response (Ostfeld, 2009; Pascual and Bouma, 2009; Randolph, 2009), [5] complex analyses to account for multiple, interdependent covariates (Dobson, 2009; Ostfeld, 2009; Pascual and Bouma, 2009, Randolph, 2009), [6] host movement in response to climate change (Harvell et al., 2009), and [7] geographic tools to account for distinctions between fundamental and realized niches (Ostfeld, 2009; Randolph, 2009)." And in light of these many and varied challenges that confront the scientific community in this emerging field of study, there is much unfinished business that needs to be conducted in researching the several potential relationships that may (or may not) exist between climatic change and the spread of infectious diseases. Hence, it should be abundantly clear that the numerous viral and vector-borne health catastrophes that are routinely predicted to occur by the world's climate alarmists in response to future global warming are definitely not yet ready for prime-time consideration, much less unquestioning acceptance.
Inching one year closer to the present, Reiter (2010) writes that the appearance of the West Nile virus in New York (USA) in 1999, plus the unprecedented panzootic that followed, "have stimulated a major research effort in the Western Hemisphere and a new interest in the presence of this virus in the Old World," which developments have been driven in part by the fact that "a great deal of attention has been paid to the potential impact of climate change on the prevalence and incidence of mosquito-borne disease." Therefore, Reiter reviews what researchers have learned about the subject and reports the worldwide implications for public health, summing things up in his final paragraph, where he states that "one point is clear: the importation and establishment of vector-borne pathogens that have a relatively low profile in their current habitat is a serious danger to Europe and throughout the world," which state of affairs, in his view, "is a direct result of the revolution of transport technologies and increasing global trade that has taken place in the past three decades," modern examples of which include "the global circulation of dengue virus serotypes (Gubler, 1998), the intercontinental dissemination of Aedes albopictus and other mosquitoes in used tires (Hawley et al., 1987; Reiter, 1998), the epidemic of chikungunya virus in Italy (Angelini et al., 2007), and the importation of bluetongue virus and trypanosomiasis into Europe (Meroc et al., 2008; Moretti, 1969)." And he further concludes that in view of what his review reveals, "globalization is potentially a far greater challenge to public health in Europe than any future changes in climate (Tatem et al., 2006)."
Last of all, writing that "pathogens cause roughly one in five human deaths, are responsible for 51% of years of life lost globally, and have long affected human demographics," Dunn et al. (2010) state that pathogens "have also been identified as drivers of human behavior, the politics and political stability of countries, human fertility, global economies, and more generally the course and dynamics of human history." And, somewhat ominously, they report that "researchers have linked the presence and prevalence of some pathogens to climate, as has been highlighted in recent discussions of climate change and disease," where they specifically mention malaria, plague and dengue as examples of the latter. Thus, they conducted, as they describe it, "a global analysis of the relative influence of climate, alternative host diversity and spending on disease prevention on modern patterns in the richness and prevalence of human pathogens."
As a result of their work, the U.S., Canadian and New Zealand researchers found that "pathogen richness (number of kinds) is largely explained by the number of birds and mammal species in a region," and that "the most diverse countries with respect to birds and mammals are also the most diverse with respect to pathogens." And noting, in this regard, that "we are unlikely to be able to change patterns of pathogen richness dramatically," they go on to state that "pathogen richness, even when high, does not guarantee high prevalence, because of the potential impact of disease control effort." In fact, they found that "pathogen prevalence is much more sensitive to variation in health spending among regions," and that "importantly, for human health, the prevalence of key human pathogens is strongly influenced by disease control efforts."
As a consequence of the above observations, Dunn et al. conclude that "even where disease richness is high, we might still control prevalence, particularly if we spend money in those regions where current spending is low, prevalence is high and populations are large." And let's be realistic about it: this approach is infinitely more likely to succeed in its worthy objectives than is the nebulous idea (i.e., the wishful thinking) of changing the planet's climate. And with all of the unanticipated consequences of such an effort -- many of which may be assumed to be negative and are almost assured to occur with the undertaking of such a huge and complex campaign -- we could well be better off to do nothing than to gamble all that the human family has achieved over the millennia, fighting a war against something so ethereal as CO2-induced global warming.




